- Blood is a special connective tissue consisting of a fluid matrix, plasma, and formed elements (Erythrocytes, leucocytes, and platelets).
- In a healthy person, approximately 5 liters (12 pints) of blood circulates throughout their body. Erythrocytes or red blood cells (RBC) are the most abundant of all the cells in the blood.
- RBCs are formed in the red bone marrow in adults. RBCs are devoid of the nucleus in most mammals and are biconcave in shape. They have a red coloured, iron-containing complex protein called hemoglobin, hence the colour and name of these cells.
- Leucocytes are also known as white blood cells (WBC) as they are colorless due to the lack of hemoglobin. They are nucleated and are relatively lesser in number which averages 6000- 8000 mm-3 of blood.
- Leucocytes are generally short-lived. We have two main categories of WBCs – granulocytes and agranulocytes. Neutrophils, eosinophils, and basophils are different types of granulocytes, while lymphocytes and monocytes are agranulocytes.
- The main function of platelets is to contribute to hemostasis: the process of stopping bleeding at the site of interrupted endothelium. They gather at the site and unless the interruption is physically too large, they plug the hole.
- Blood
- Blood accounts for 7% of body weight.
- An average adult has a blood volume of roughly 5 litres.
- Blood cell- RBC-45%, Plasma- 54.3% and WBC-0.7%
- Note: Plasma, which is 92 percent water, constitutes 55 percent of blood volume. Plasma contains albumin (the chief protein constituent), fibrinogen (responsible, in part, for the clotting of blood), and globulins (including antibodies).
Blood Groups: ABO Blood Group and Rh Group System
Even though components of blood are the same for all humans, there are various blood types. In fact, there are more than 40 blood groups, but all of them are not clinically significant. The discovery of the ABO blood group created great excitement as until then, all blood had been assumed to be the same.
Karl Landsteiner, an Austrian scientist discovered the ABO blood group system in the year 1900.
There are four principal types: A, B, AB, and O.
There are two antigens and two antibodies that are mostly responsible for the ABO types. The specific combination of these four components determines an individual’s type in most cases.
The table below shows the possible permutations of antigens and antibodies with the corresponding ABO type (“yes” indicates the presence of a component and “no” indicates its absence in the blood of an individual).
| ABO Blood Type | Antigen A | Antigen B | Antibody Anti-A | Antibody Anti-B |
| A | yes | no | no | yes |
| B | no | yes | yes | no |
| O | no | no | yes | yes |
| AB | yes | yes | no | no |
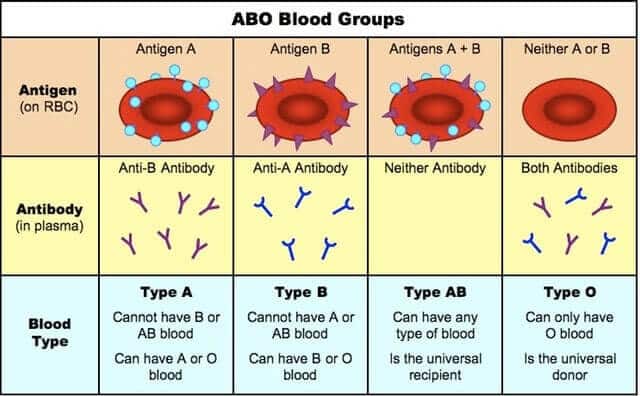
For example, people with type A blood will have the A antigen on the surface of their red cells (as shown in the table below). As a result, anti-A antibodies will not be produced by them because they would cause the destruction of their own blood.
However, if B type blood is injected into their systems, anti-B antibodies in their plasma will recognize it as alien and burst or agglutinate the introduced red cells in order to cleanse the blood of alien protein.
| ABO Blood Type | Antigen A | Antigen B | Antibody Anti-A | Antibody Anti-B |
| A | yes | no | no | yes |
| B | no | yes | yes | no |
| O | no | no | yes | yes |
| AB | yes | yes | no | no |
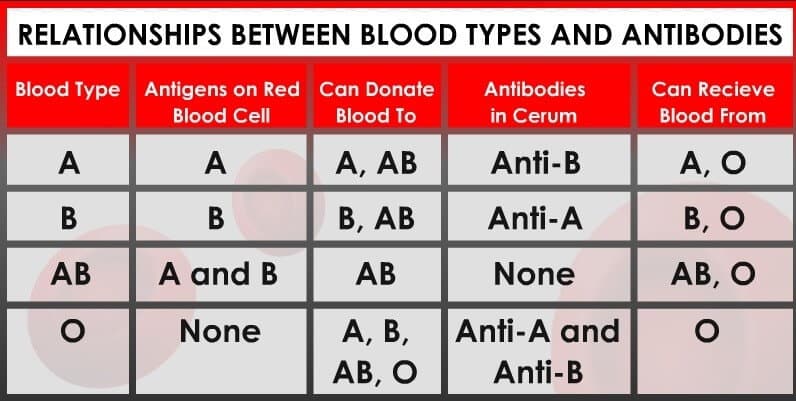
Individuals with type O blood do not produce ABO antigens.
- Therefore, their blood normally will not be rejected when it is given to others with different ABO types.
- As a result, type O people are universal donors for transfusions, but they can receive only type O blood themselves.
Those who have type AB blood do not make any ABO antibodies.
- Their blood does not discriminate against any other ABO type.
- Consequently, they are universal receivers for transfusions, but their blood will be agglutinated when given to people with every other type because they produce both kinds of antigens.
| ABO Blood Type | Antigen A | Antigen B | Antibody Anti-A | Antibody Anti-B |
| A | yes | no | no | yes |
| B | no | yes | yes | no |
| O | no | no | yes | yes |
| AB | yes | yes | no | no |
- It is easy and inexpensive to determine an individual’s ABO type from a few drops of blood. A serum containing anti-A antibodies is mixed with some of the blood. Another serum with anti-B antibodies is mixed with the remaining sample.
- Whether or not agglutination occurs in either sample indicates the ABO type.
- It is a simple process of elimination of the possibilities. For instance, if an individual’s blood sample is agglutinated by the anti-A antibody, but not the anti-B antibody, it means that the A antigen is present but not the B antigen. Therefore, the blood type is A.
Rh Blood Group System
- In addition to the ABO blood grouping system, the other prominent one is the Rh blood group system.
- About two-thirds of the population (nearly 80 percent) contains the third antigen on the surface of their red blood cells known as the Rh factor or Rh antigen; this decides whether the blood group is positive or negative.
- If the Rh factor is present, an individual is rhesus positive (Rh+ve);
- if the Rh factor is absent individual is rhesus negative (Rh-ve) as they produce Rh antibodies.
- An Rh-ve person, if exposed to Rh+ve blood, will form specific antibodies against the Rh antigens. Therefore, the Rh group should also be matched before transfusions.
- A special case of Rh incompatibility (mismatching) has been observed between the Rh-ve blood of a pregnant mother with Rh+ve blood of the foetus.
- Rh antigens of the foetus do not get exposed to the Rh-ve blood of the mother in the first pregnancy as the two bloods are well separated by the placenta.
- However, during the delivery of the first child, there is a possibility of exposure of the maternal blood to small amounts of the Rh+ve blood from the foetus.
- In such cases, the mother starts preparing antibodies against Rh antigen in her blood.
- In case of her subsequent pregnancies, the Rh antibodies from the mother (Rh-ve) can leak into the blood of the foetus (Rh+ve) and destroy the foetal RBCs.
- This could be fatal to the foetus or could cause severe anaemia and jaundice to the baby. This condition is called erythroblastosis foetalis.
- This can be avoided by administering anti-Rh antibodies to the mother immediately after the delivery of the first child.
